What is heart blockage:
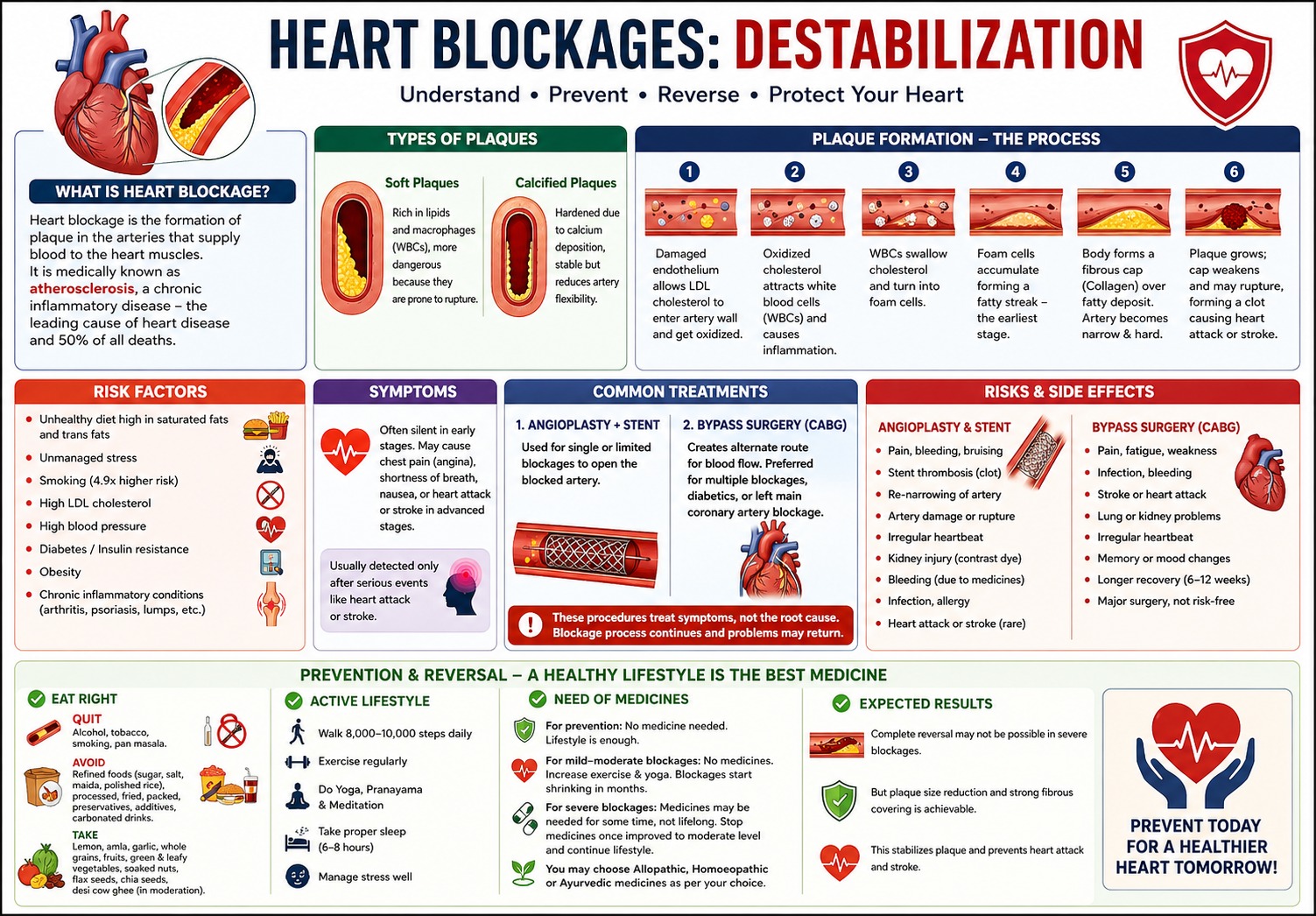
Heart blockage is the formation of plaque/s in the inner wall of the arteries of the heart that supply blood to the heart muscles. In medical terms this is known as atherosclerosis, a chronic inflammatory disease — that causes 50% of all deaths and is considered the major cause of all cardiovascular diseases.
Composition of plaques:
Plaque is a complex mixture of lipids (LDL cholesterol and triglycerides), cellular waste products, calcium, fibrin, and other debris that slowly builds up in artery walls over a long period of time, and its composition shifts towards higher lipid accumulation as the plaque progresses.
Types of plaques:
Soft plaques – rich in lipids and macrophages (WBCs), more dangerous because they are prone to rupture.
Calcified plaques: hardened due to calcium deposition, which stabilizes them but restricts artery flexibility.
What causes plaque formation:
Our entire blood vessels have a thin, single layer of specialized cells, known as endothelium. This layer is considered the brain of the blood vessels. It is a dynamic, single-cell lining of arteries that acts as a vital, active organ. It produces nitric oxide (NO), the most vital chemical that makes blood vessels flexible and stretchable, which is crucial to keep blood pressure under control. When the endothelium does not get the right nutrition, it becomes dysfunctional, damaged, or permeable and creates room for plaque formation.
How plaques are formed:
- Dysfunctional and damaged endothelial lining of the artery permits LDL cholesterol to enter the vessel wall and get stuck there. Over time, it becomes oxidized and damaged.
- This damaged cholesterol sends signals that attract white blood cells (the body’s immune cells) to that spot. As a defense mechanism, WBCs initiate inflammation.
- These white blood cells try to clean up by swallowing the damaged cholesterol. After taking in too much cholesterol, they turn into “foam cells,” which are filled with fat.
- When these fat-filled cells (called foam cells) build up inside the blood vessel wall, they form a thin, yellowish layer called a fatty streak. This is the earliest stage of blockage in the arteries.
- The body tries to protect the damaged area. It sends special cells that create a covering (like a patch) made of strong fibers (collagen). This covering is called a fibrous cap, and it forms over the fatty deposit. Consequently, the artery becomes narrow and harder, restricting normal blood flow. This stage may last for years silently without showing any symptom.
- Over time, this fatty buildup (plaque) becomes larger. Sometimes, the covering (fibrous cap) becomes weak and gets ruptured. When this happens, a blood clot can form, which may block blood flow suddenly, leading to a heart attack or stroke.
RISK FACTORS:
- Regular intake of unhealthy diet high in saturated fats and trans-fatty acids that lacks nitrate, a precursor of nitric oxide.
- Unmanaged or inadequately managed stress.
- Smoking, which carries a 4.9 times higher risk of significant plaque volume.
- High levels of low-density lipoproteins (LDL cholesterol).
- High blood pressure, the very first signal of a damaged arterial wall (endothelium).
- Diabetes/insulin resistance: plaque burden 48.34% in diabetics vs. 33.01% in non-diabetics.
- Chronic inflammatory conditions like lumps, arthritis, psoriasis, etc.
SYMPTOMS: This is an asymptomatic disease that usually produces no symptom in the developing stage. It can begin as early as childhood (thanks to junk food culture) and progress slowly, generally increasing in severity with age. With sufficient progression it can lead to chest pain (angina), dyspnea, nausea, or severe cardiac events and is often detected only after a person has had a heart attack or stroke.
Most common treatment given:
- Angioplasty + stent: given in case of single or limited blockages to open a blocked artery.
- Bypass surgery (CABG): done to create alternate blood flow. CABG is preferred in case of multiple blockages, diabetics, or blockage/s in the left main coronary artery.
Efficacy of these invasive procedures:
None of these procedures address the root cause of plaque buildup and simply treat the symptoms of advanced plaque buildup, with the result that the process of plaque buildup continues as such, and after a few years symptoms redevelop and these procedures are repeated again and again. Moreover, in most cases these procedures are done after the person gets a heart attack or stroke, i.e. after the person has suffered one of the worst possible harms of arterial plaques.
Side effects and risks of angioplasty and stents:
Common side effects
- Pain or discomfort at the catheter insertion site (groin/arm)
- Minor bleeding or bruising
- Temporary chest discomfort
- Need for lifelong medication
Risks / complications
- Stent thrombosis (dangerous clot inside stent)
- Artery re-narrowing (restenosis)
- Artery damage or rupture
- Irregular heart rhythm (arrhythmia)
- Kidney injury (due to contrast dye)
- Allergic reaction (to metal or drug coating)
- Bleeding risk (due to antiplatelet medicines)
- Infection – Rare
- Heart attack or stroke – Rare
Limitations:
- Not suitable for multiple or complex blockages
- Lifelong medication compliance required
- Risk increases if medicines are stopped
Side effects and risks of bypass surgery (CABG)
Common side effects:
- Pain at chest incision site
- Fatigue and weakness (weeks to months)
- Swelling in legs (if vein graft used)
- Breathing tube in the throat (for some time)
- Loss of appetite
- Severe Shortness of breath
- Difficulty sleeping or mood changes
Risks / complications
- Infection (chest wound or graft site)
- Bleeding or need for transfusion
- Stroke or heart attack
- Memory loss or cognitive decline (temporary in many)
- Lung complications
- Kidney dysfunction
- Irregular heart rhythm (especially atrial fibrillation)
Limitations
- Major surgery with longer recovery (6–12 weeks)
- Not risk-free
PREVENTION & REVERSAL:
Atherosclerosis, as well as its triggers (blood pressure, blood sugar, cholesterol, triglycerides, stress, etc.), can be very well prevented and, in majority of cases, significantly improved by adopting a healthy lifestyle.
Diet:
- Quit: alcohol, tobacco, smoking, pan masala.
- Avoid: refined food items (Sugar, Salt, Maida, Refined Oils, Polished rice and dals), processed and packed food items, fried food, refrigerated food, foods/drinks, carbonated drinks, items having preservatives, additives, and chemicals.
- Take: lemon, amla, garlic, whole grain with bran, coarse grains with bran, seasonal fruits, green vegetables, leafy vegetables, soaked nuts (almonds, walnuts), flax seeds, chia seeds, healthy fat (desi cow ghee) in proportion to the physical activities you usually undertake.
- Walk (8,000–10,000 steps) daily, exercise, do yoga, pranayama, and meditation (video and/or description of these are being added to our website shortly).
- Take proper sleep (6–8 hours).
- Manage your stress well. If need be consult for stress management.
- Need of medicines:
- For prevention, no medicine is required; lifestyle measures are enough to remain free of all lifestyle diseases.
- For minor to moderate blockages also, no medicines are required; just slightly increase the duration and intensity of exercises, yoga, etc. Within a few months, blockages will start to shrink and the covering will become harder, keeping you safe from heart attack and stroke.
- In severe blockages, medicines may be necessary for some time (not lifelong). Lifestyle measures take some time to begin their effects. Once blockages have shrunk to a moderate level, medicines may be stopped while lifestyle measures are kept
- You may take either allopathic, homoeopathic, or ayurvedic medicines as per your choice. Due to the side effects of allopathic medicines we prefer homoeopathic or ayurvedic medicines, or even both which are equally effective.
Expected results:
- In case of severe blockages, complete reversal may not be difficult (not impossible), but size reduction and development of a tough covering, making the plaque stable to prevent rupture and complications, can definitely be expected.
For details visit us : www.swasthyabhandar.com>Diseases & consultancy>some diseases>cardiovascular diseases.